
'Mud fever' is a common name for pastern dermatitis and contrary to popular belief, it is not a specific disease. Mud fever is actually a collection of factors and diseases that contribute to irritation, damage and infection of the skin on the lower limbs of horses. However, the most common causative organism is indeed one strain of bacteria, Dermatophilus congolensis, which is believed to live in mud and is also found naturally on the skin. That said, the bacterium is unable to penetrate the skin's surface so it must be weakened first and this is where the wet weather and muddy conditions raise it's prevalence during autumn and winter months.
The skin is an animal's largest organ and together with its appendages, such as sebaceous glands and hair, makes up the integumentary system that primarily serves to protect the body from the outside world. The skin has a far more complicated structure than formerly thought, enabling it to perform its regulatory and protective roles. The outermost layer of skin is specially adapted to serve as the 'frontline' of an animal's defences and even has an acidic layer to prevent microbial colonisation. Nevertheless, there are various factors that contribute to the breakdown of this barrier.
 Unfortunately in England, the weather contributes to a vast majority of skin related problems and with wet conditions stretching through our summers, incidence of mud fever is high with devastating consequences for our equine friends! When the skin is exposed to wet conditions for prolonged periods of time, the outermost layer which usually has a low percentage of water in its cells, absorbs a significant amount of water causing swelling and pronounced softening of the skin.
Unfortunately in England, the weather contributes to a vast majority of skin related problems and with wet conditions stretching through our summers, incidence of mud fever is high with devastating consequences for our equine friends! When the skin is exposed to wet conditions for prolonged periods of time, the outermost layer which usually has a low percentage of water in its cells, absorbs a significant amount of water causing swelling and pronounced softening of the skin.
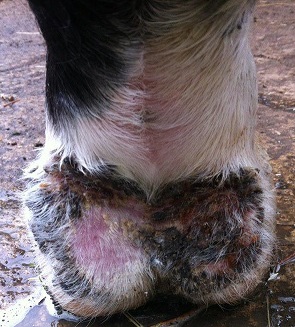
When the skin is in this state and particularly if the lower limbs are repeatedly dried and re-exposed to damp conditions, the protective barrier becomes greatly weakened. Often, small splits along the heels are the first lesions to appear and allow entry of skin and mud-dwelling bacteria. Crusty scabs will appear around the heels and if left, the condition will worsen, spreading further and deeper into the tissues. The most severe cases see deep cracks along the heels, pus filled wounds and inflammation that lead to lameness. In some cases the infection may travel up the legs. Dermatophilus congolensis is a particular type of bacteria that behaves both like a bacterium and a fungus. It often lies dormant on the skin or lives in the soil feeding on organic matter and when its spores come into contact with deficient skin barriers, they are able to invade the skin with hyphae (long, finger-like projections) and cause the initial inflammatory reaction. While Dermatophilus is a common cause, many other factors including contact dermatitis (allergies), irritants, and Chorioptic mange mites are often involved in damaging the protective barrier and contribute toward infection by other bacteria and fungi, producing mud fever symptoms.
There are two important conditions that may predispose a horse to Mud Fever but they are frequently overlooked. The first is Pastern Leukocytoclastic Vasculitis (PLV), usually seen to affect the blood vessels in areas of skin lacking pigment, such as the skin beneath white socks. It is thought to be an immune-mediated condition although it does involve some photosensitivity where UV light causes a reaction that weakens the skins integrity. The second is Chronic Progressive Lymphedema (CPL), a condition that affects certain breeds of horse, usually draft breeds such as Clydesdales. The problem lies within the lymphatic system, where fluid does not drain back into the vessels and builds within the tissues and secondary infections are common. The long feathers on the heels of such breeds hide the early signs of disease but also trap mud and water, further increasing the risk that the horses will develop Mud Fever at some point in their lives. The two conditions both require a biopsy for proper diagnosis and veterinary treatment, although animals with CPL must be managed long term to ensure a better quality of life throughout the disease progression.
Ease of treatment ranges along with severity of the disease and possible underlying symptoms. The surrounding hair is often clipped away first to allow better air circulation so that the moisture is not retained and to allow topical treatments to be applied more successfully. Generally, the aim is to gently soak and peel off the scabs and then clean the wounds with a warm, diluted disinfectant such as Hibiscrub (Chlorhexidine gluconate) or Vetasept (Povodine-Iodine). These products will also protect the wound against further infection and can be left on to penetrate the sores for a few minutes before rinsing.
After removing the shallower scabs and washing, the legs should be dried with a clean cloth or possibly a hair dryer if your horse will tolerate the noise. It is best to leave the legs to air whenever possible, rather than applying a dressing which will retain moisture and promote proliferation of the infectious organism. When the legs are dry, topical antiseptic creams such as Dermisol can be applied to the wounds to aid healing and provide protection against potential invaders.
This will all need to be repeated for several days until the infection has cleared up and wounds have healed. Gentle exercise on dry ground can be undertaken but an affected horse should be stabled in the dry and away from its companions until the wounds have healed. Alternatively, if you have a dry field or manège, your horse can be turned out there. Grooming equipment and boots should not be shared with infected animals and handlers must always wash their hands thoroughly after treating wounds and between touching another horse- the infection can spread to both other horses and humans.
Removal of thicker scabs is often painful and usually requires sedation by a vet but it is vital to allow topical treatments to reach the causative organism. Veterinary attention will be required for the more advanced cases and for those which do not clear up and prescription only treatments will be needed to clear infection from the body and help heal the wounds. If your horse is found to have another contributory condition, your vet will help you to either resolve it or manage it. It is advisable to keep a close eye on any horse who has experienced mud fever, as their skin may be more susceptible to recurrent infection upon return to the field.
After looking at the causes and treatments for mud fever, it is easy to conclude that every reasonable step should be taken to prevent it! While the minority of horses will have a difficult underlying condition to address, the majority of cases can and should be avoided.
 Firstly, have a look at the field your horse is turned out into. If it has boggy or very muddy areas, fence these off and if you have multiple paddocks, rotate them. When you bring your horse in, their stable should be well-ventilated and dry. Conforming to good stable management and ensuring damp bedding is replaced daily will play a role in preventing irritation and infection of the skin on the heels. Brushes, bandages, wraps and boots should not be swapped between animals, especially if a horse is prone to or suffering from mud fever. Equipment and stables should be washed and disinfected regularly.
Firstly, have a look at the field your horse is turned out into. If it has boggy or very muddy areas, fence these off and if you have multiple paddocks, rotate them. When you bring your horse in, their stable should be well-ventilated and dry. Conforming to good stable management and ensuring damp bedding is replaced daily will play a role in preventing irritation and infection of the skin on the heels. Brushes, bandages, wraps and boots should not be swapped between animals, especially if a horse is prone to or suffering from mud fever. Equipment and stables should be washed and disinfected regularly.
Before exercise and turn out, use a topical barrier cream such as those designed by Lincoln, Net-Tex and NAF. Topical products will play a huge role in preventing mud fever as they create a waterproof and antimicrobial barrier between the horse's skin and the environment. After exercise and turn out, do not hose down a horse's feet every day. Wait for the mud to dry and then use a soft brush to remove the dried mud. This reduces the risk of scratching vulnerable skin and prevents excess wetting and related damage from over-washing.
Waterproof leg wraps and boots can be very helpful for susceptible horses as they provide another physical barrier to keep the mud and water off of the skin and prevent scrapes in the field. Nutritional supplements can be considered to encourage and maintain healthy skin to better resist or recover from damage in wet conditions.
Finally, carefully checking your horse's heels and legs daily will allow you to spot any early signs of trouble. Be sure to wash and treat any small grazes or cuts immediately to prevent infection and take extra time when checking horses with long heel feathers, as signs are often harder to find.
It turns out that 'Mud Fever' isn't always a simple condition with a simple answer. The focus should be on future prevention. The general consensus is that your horse should be kept out of the mud. Yes, prolonged periods in wet conditions should be avoided and many infections will be a result of mud related pathogens -hence the name 'Mud Fever'- but you should also be looking out for other conditions or parasites that can affect your horse's risk of acquiring it and address these with the help of your vet. Don't be shy about asking for help or for a second opinion and always act as soon as you detect a potential problem. There are wide ranges of effective products to protect your horse's legs and help wounds heal, and should you ever need some advice on which ones to use, you can of course contact us at VioVet.